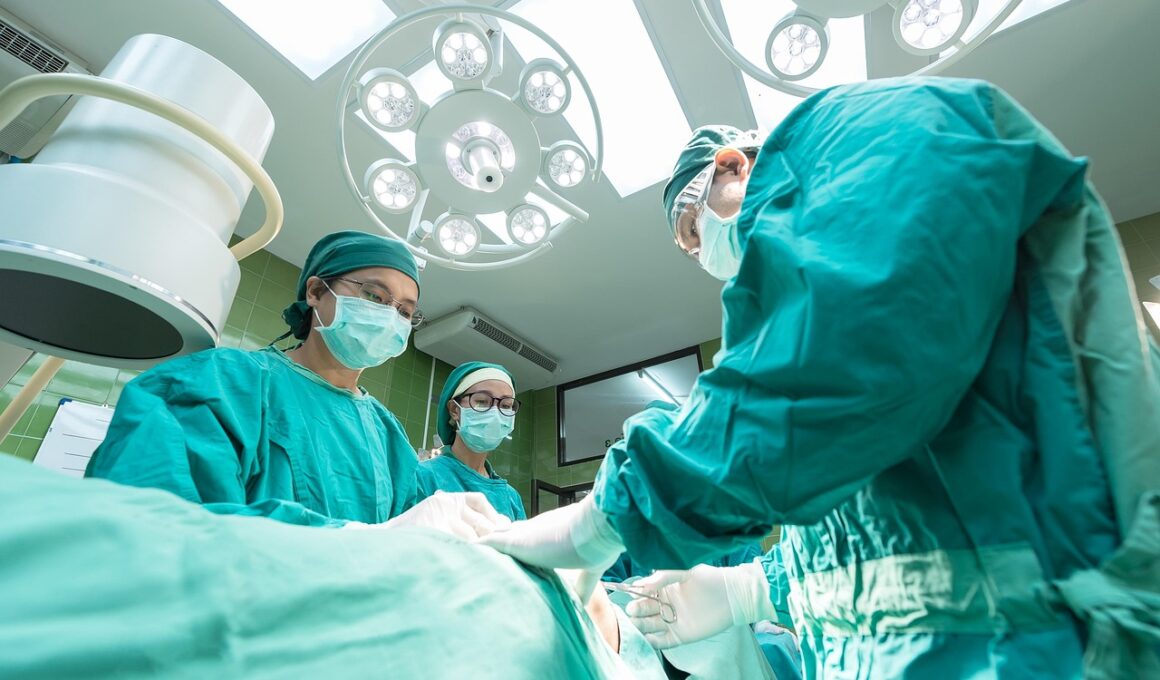
Streamlining Emergency Department Operations with Lean Tools
The implementation of Lean Management techniques in healthcare settings can significantly enhance operational efficiency, particularly in emergency departments (EDs). These departments often face challenges such as overcrowding, long wait times, and resource constraints. By adopting Lean principles, healthcare providers can minimize waste, streamline processes, and optimize patient flow. Lean allows teams to identify unnecessary steps in workflows and refine them to improve service delivery. Key tools, including Value Stream Mapping, can help visualize patient journeys, identify bottlenecks, and foster improvements. Implementing Lean in the ED not only enhances patient care but also staff satisfaction as their workflows become more manageable and less chaotic. Training staff on Lean methodologies equips them to identify inefficiencies proactively and suggest improvements. Ultimately, the goal is to create a more responsive and effective emergency department. As such, the commitment must also come from leadership, which is crucial for fostering a culture of continuous improvement. Communication across departments can aid in the collaborative efforts needed to streamline processes and encourage shared responsibility for patient outcomes. This holistic approach will go a long way in transforming ED operations to meet increasing patient demands.
One of the essential Lean tools that can transform operations in emergency departments is the 5S methodology. This technique encourages creating and maintaining a tidy work environment to promote efficiency. The five components of 5S—Sort, Set in Order, Shine, Standardize, and Sustain—help staff organize their workspace effectively. By systematically categorizing and prioritizing equipment and supplies, emergency personnel can reduce the time spent searching for critical items during a crisis. Doing so decreases waste and improves response times, positively impacting patient outcomes. Implementing 5S also engages team members, fostering a collaborative spirit focused on the shared objective of excellent patient care. Beyond the physical workspace, fostering a 5S mindset cultivates a culture of care and attention to detail among staff. Additionally, conducting regular audits ensures maintenance and adherence to the 5S practices. With ongoing training and reinforcement, teams can sustain these improvements long-term, making them integral to the department’s operations. Establishing clear metrics to evaluate the impact of these changes allows leaders to assess progress and make necessary adjustments. Continuous evaluation ensures that Lean principles adapt to evolving workflows and patient needs, making them vital tools for the ED.
Reducing Patient Wait Times
Another key focus of Lean in emergency departments is reducing patient wait times. Long waits can lead to patient dissatisfaction and may even worsen medical outcomes. Utilizing tools such as Kaizen events can help identify and resolve specific bottlenecks in care delivery. These events involve teams coming together to analyze current conditions, brainstorm solutions, and implement changes within a short timeframe. By engaging frontline staff in this process, insights are leveraged that management may overlook. Strategies may include reorganizing staff roles, modifying triage processes, or adjusting shift patterns to enhance service delivery. Measuring the impact of these interventions is crucial for assessing effectiveness. Metrics should be tracked, including average wait times and patient satisfaction scores, to evaluate the implemented changes. Additionally, it is vital to communicate findings back to the team, fostering a sense of ownership and accountability. Celebrating successful improvements reassures staff that their efforts lead to positive changes, ensuring ongoing engagement. Ultimately, these initiatives contribute to a more efficient emergency department that effectively addresses community health needs, fostering a culture of continuous improvement and excellence in patient care.
Effective communication is another cornerstone of Lean management within emergency departments. Patient flow relies heavily on the coordination between various team members, from physicians to nurses, administrative staff, and ancillary services. Lean practices advocate for standardized communication protocols designed to eliminate misunderstandings and ensure everyone is on the same page. These protocols can be facilitated through regular huddles or briefings at the start of shifts, where team members can discuss patient statuses, anticipated challenges, and daily goals. Emphasizing collaborative approaches can significantly enhance patient care and operational efficiency. Tools such as Checklists and Visual Management Boards can help in maintaining clarity and focus on priorities among staff. Another aspect is utilizing technology for real-time updates on patient movements and statuses. Electronic health records (EHR) systems, for example, can aid in tracking a patient’s journey through the ED. By promoting transparency and information sharing, the whole team remains engaged and accountable for their roles in patient care. Continuous training ensures everyone understands their communication roles and responsibilities, paving the way for a more integrated approach to care management.
Empowering Staff Through Training
Implementing Lean tools effectively involves empowering staff through targeted training programs. Educational initiatives need to focus not only on Lean principles but also on practical applications tailored to their specific roles within the ED. Workshops, simulations, and hands-on training can bring the concepts to life, making them relevant to daily operations. Encouraging staff to participate in these training sessions fosters a sense of ownership and accountability, thereby promoting a culture of continuous improvement. Staff engagement is crucial; they can provide valuable insights about processes, patient interactions, and best practices that can further streamline operations. Fostering this partnership not only enhances knowledge but also builds trust among team members. Engaged staff are more likely to suggest improvements based on their experiences, which can lead to innovative solutions to existing challenges. Moreover, ongoing training ensures that teams adapt swiftly to changes and develop resilience as the department evolves with increasing patient demands. As a result, investing in staff training not only improves individual capabilities but also creates a more cohesive and effective team working towards optimizing patient care in the emergency department.
Utilizing technology alongside Lean principles can significantly enhance emergency department operations. Implementing advanced software systems for tracking patients can help manage workflows more effectively, reducing bottlenecks caused by delays in information transfer. Technologies such as real-time tracking and predictive analytics have been integral in streamlining processes. These systems can analyze historical data to forecast peak arrival times and patient acuity levels, leading to more effective staffing and resource allocation. Additionally, technology aids in improving patient registration and intake processes, allowing for quicker transitions from arrival to treatment. Digital solutions can also support remote consultations, decreasing the immediate load on the ED while providing timely care. Furthermore, integrating patient feedback mechanisms through apps can enhance service delivery by identifying areas needing improvement. Technology can thus complement Lean strategies, providing a more streamlined patient experience. As departments embrace technological advancements, the synergy created between Lean tools and digital solutions leads to comprehensive workflow optimization. Continuous adaptation to these technologies ensures emergency departments remain responsive to community healthcare needs while safeguarding quality standards in patient care.
Measuring Success in Lean Implementation
Finally, measuring the success of Lean implementation is crucial for recognizing areas of strength and opportunities for improvement in emergency department operations. Establishing key performance indicators (KPIs) can help track progress on various fronts, including patient wait times, treatment times, and overall satisfaction scores. Regularly reviewing these metrics allows teams to assess how initiatives impact operational efficiency and patient care quality. Tools like dashboards can visualize these statistics, making it easier for departments to keep track of their performance. Involving all team members in these assessments is essential for fostering accountability and collaboration. Engaging staff in evaluating success not only demonstrates the outcomes of their efforts but also promotes a sense of ownership over improvements. Gathering qualitative feedback from patients can provide additional context to the quantitative data gathered, allowing for more targeted enhancements in operations. Lean implementation is not a one-time event but an ongoing process of refinement and adaptation. Creating a culture of continuous evaluation ensures that emergency departments respond effectively over time. Ultimately, a commitment to tracking improvements strengthens Lean’s impact on healthcare delivery and encourages sustained quality in patient care.
In conclusion, Lean principles offer various tools and strategies for optimizing emergency department operations. By focusing on waste reduction, enhancing communication, and implementing staff training programs, EDs can significantly improve their performance metrics and overall patient care experience. Technology plays a vital role in this transformation and should be seen as an ally in the journey towards making healthcare more efficient. As departments embrace Lean practices and commit to continuous improvement, they ultimately foster a culture of excellence that resonates throughout the organization. Engagement from all team members, including leadership support, is crucial for the long-term success of implementing these methodologies. Continuous assessments through KPIs provide a roadmap for future enhancements, ensuring that EDs are always striving for improvement. Adapting to ever-evolving challenges allows departments to remain not only responsive but also proactive in addressing community health needs. As healthcare environments continue to change, Lean principles will serve as efficient tools for navigating those challenges ahead. The dedication to streamlining operations reinforces the commitment to delivering high-quality patient care. With Lean practices embedded in daily operations, emergency departments can better fulfill their vital role in the healthcare ecosystem.